Face transplants can take as long as 25 hours, but surgeons typically have one hour to attach the vascular connections from the donor face to the recipient. During this time, the patient's blood flow is stopped. Adequate preparation is crucial, and researchers and physicians at Brigham and Women's Hospital in Boston increasingly turn to 3D printing to help ensure a successful outcome.
December 2, 2014
Face transplants can take as long as 25 hours, but surgeons typically have one hour to attach the vascular connections from the donor face to the recipient. During this time, the patient's blood flow is stopped. Adequate preparation is crucial, and researchers and physicians at Brigham and Women's Hospital in Boston increasingly turn to 3D printing to help ensure a successful outcome. A study on the use of 3D-printed life-size models of patients' heads to assist in face-transplant surgery was presented at the annual meeting of the Radiological Society of North America (RSNA), currently underway in Chicago.
In the study, a research team led by Frank J. Rybicki, MD, radiologist and director of the hospital's Applied Imaging Science Laboratory; Bohdan Pomahac, MD, lead face transplantation surgeon; and Amir Imanzadeh, MD, research fellow, assessed the clinical impact of using 3D-printed models of the recipient's head in the planning of face-transplantation surgery.
"This is a complex surgery, and its success is dependent on surgical planning," Rybicki said. "Our study demonstrated that if you use this model and hold the skull in your hand, there is no better way to plan the procedure."
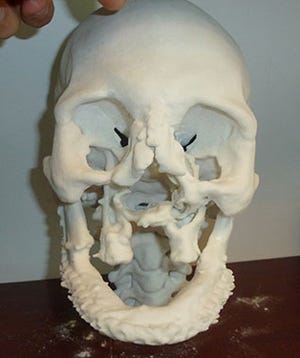 To build each life-size skull model, preoperative computed tomography (CT) images of the patient's head were processed using custom software, creating specialized data files that were input into a 3D printer.
To build each life-size skull model, preoperative computed tomography (CT) images of the patient's head were processed using custom software, creating specialized data files that were input into a 3D printer.
During a press conference at the meeting, Rybicki discussed the impact of Stratasys (Minneapolis, MN) 3D printing for soft tissue in one transplant patient. "We've 3D printed the soft tissues before and after [the patient's] full-face transplantation," said Rybicki in a news release from Stratasys. "We're going to illustrate those dramatic changes in tissues using a new method that has been previously unavailable. The soft tissues that are 3D printed in one piece are much better than photographs. They provide a better understanding of what's between the skin and bones than any two-dimensional representation can," he said.
The models were created using Stratasys Objet500 Connex3 and Objet Eden 260VS 3D printers.
Explaining the value of 3D printing in improving patient care, Imanzadeh told RSNA attendees that the patient's facial bones sometimes need to be modified prior to transplantation. "The 3D-printed model helps us to prepare the facial structures so when the actual transplantation occurs, the surgery goes more smoothly," said Imanzadeh.
"If there are absent or missing bony structures needed for reconstruction, we can make modifications based on the 3D-printed model prior to the actual transplantation, instead of taking the time to do alterations during ischemia time [when blood flow is stopped]," Rybicki added.
The researchers said they also used the models in the operating room to increase surgeons' understanding of the anatomy of the recipient's face during the procedure.
"You can spin, rotate, and scroll through as many CT images as you want, but there's no substitute for having the real thing in your hand," Rybicki said. "The ability to work with the model gives you an unprecedented level of reassurance and confidence in the procedure."
Based on the results of this study, 3D printing is now routinely used for surgical planning for face-transplantation procedures at Brigham and Women's Hospital, and 3D-printed models may be implemented in other complex surgeries.
About the Author(s)
You May Also Like


