A new injectable polymer developed by researchers at the University of Washington (UW; Seattle) could strengthen blood clots and save countless lives on the battlefield, in rural areas and anywhere else where immediate medical treatment may not be available.Following an injury, PolySTAT could be injected into the patient on site to staunch bleeding until he or she can receive proper medical care. Unlike other clotting treatments that require refrigerated or frozen blood products, a syringe loaded with the polymer could be carried inside a backpack for emergency use.
March 11, 2015
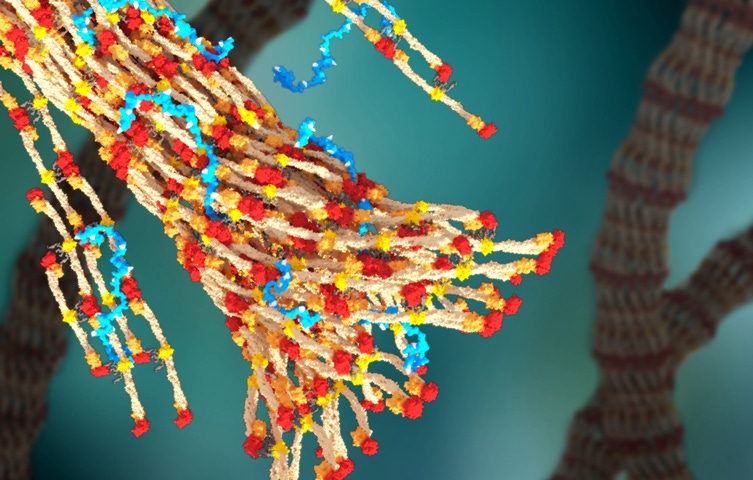
A new injectable polymer developed by researchers at the University of Washington (UW; Seattle) could strengthen blood clots and save countless lives on the battlefield, in rural areas and anywhere else where immediate medical treatment may not be available.
Following an injury, PolySTAT could be injected into the patient on site to staunch bleeding until he or she can receive proper medical care. Unlike other clotting treatments that require refrigerated or frozen blood products, a syringe loaded with the polymer could be carried inside a backpack for emergency use.
"Most of the patients who die from bleeding die quickly," said Dr. Nathan White, an assistant professor of emergency medicine who teamed with UW bioengineers and chemical engineers to develop the macromolecule. "This is something you could [. . . ] give right away to reduce blood loss and keep people alive long enough to make it to medical care," he said. The new polymer is described in a paper featured on the cover of the March 4 issue of Science Translational Medicine.
|
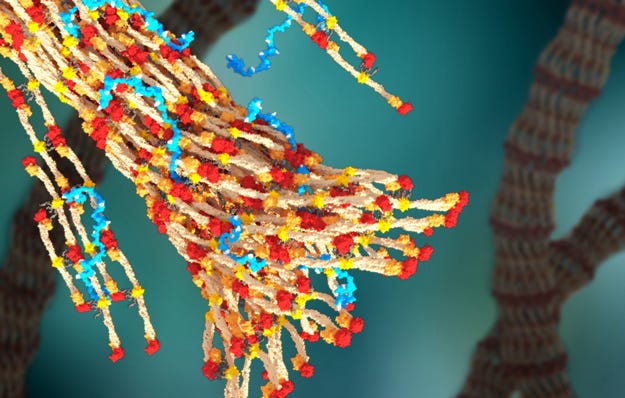
A 3D rendering of fibrin forming a blood clot, with PolySTAT (in blue) binding strands together. Graphic courtesy William Walker/University of Washington. |
In an initial study conducted with rats, 100% of animals injected with PolySTAT survived a typically lethal injury to the femoral artery. Only 20% of rats treated with a natural protein that helps blood clot survived. Researchers say that the material could reach human clinical trials in five years.
The polymer was inspired by factor XIII, a natural protein found in the body that helps strengthen blood clots, according to a news release published by UW. Following an injury, platelets in the blood begin to congregate at the wound and form an initial barrier. Then a network of specialized fibers—called fibrin—start weaving themselves throughout the clot to reinforce it, writes UW reporter Jennifer Langston. If the scaffolding can't withstand the pressure of blood pushing against it, the clot breaks apart and the patient keeps bleeding. Both PolySTAT and factor XIII strengthen clots by crosslinking fibrin strands. "It's like the difference between twisting two ropes together and weaving a net," said Suzie Pun, UW Robert J. Rushmer Professor of Bioengineering and a co-author of the paper. "The crosslinked net is much stronger."
PolySTAT has other advantages. Enzymes that typically cut fibrin strands don't target synthetic PolySTAT bonds that are integrated into the clot, keeping blood clots intact during critical hours after an injury.
The material also is potentially less expensive than currently used blood-based products that require careful storage, and it may have a lower risk profile, since it is less likely to grow bacteria or carry infectious disease.
Research indicates that PolySTAT works to strengthen clots even in cases where fibrin building blocks are critically low.
The UW team also used a highly specific peptide that only binds to fibrin at the wound site. It does not bind to a precursor of fibrin that circulates throughout the body. That means PolySTAT shouldn't form dangerous clots that can lead to a stroke or embolism.
Next steps involve testing on larger animals and additional screening to find out if PolySTAT binds to any other unintended substances. Researchers also plan to investigate the polymer's potential for treating hemophilia and for integration into bandages.
About the Author(s)
You May Also Like